
Osteoporosis prevention is crucial for maintaining strong bones and overall health as we age. By understanding the key factors that contribute to bone density, such as nutrition, exercise, and lifestyle choices, we can take effective steps to minimize the risk of this common condition. Whether it’s ensuring adequate calcium and vitamin D intake or incorporating weight-bearing exercises into our routines, proactive measures can make a significant difference.
This discussion will delve into essential strategies for osteoporosis prevention, highlighting the importance of dietary choices, the impact of lifestyle habits like smoking and alcohol consumption, and the role of healthcare in promoting awareness and early detection. By taking an informed approach, we can empower ourselves and our communities to foster better bone health.
Osteoporosis Prevention Strategies
Osteoporosis is a condition characterized by weakened bones, increasing the risk of fractures and breaks. To combat this silent disease, it’s crucial to adopt effective prevention strategies. By focusing on adequate nutrient intake, engaging in appropriate exercise, and making dietary choices that support bone health, individuals can significantly reduce their risk of developing osteoporosis.Calcium and vitamin D play vital roles in maintaining bone density and strength.
Calcium is the primary mineral found in bones, and an adequate intake is essential for bone formation and maintenance. Vitamin D is equally important as it aids in calcium absorption in the gut and helps regulate calcium levels in the blood. Without enough vitamin D, bones can become brittle and weak. To ensure optimal bone health, adults should aim for a daily intake of 1,000 to 1,200 mg of calcium and 600 to 800 IU of vitamin D, depending on age and gender.
Exercise Routines That Strengthen Bones and Enhance Balance
Regular physical activity is crucial for strengthening bones and enhancing balance, both of which are essential to prevent falls and fractures associated with osteoporosis. Weight-bearing and resistance exercises are particularly beneficial for bone health. Here are some effective exercise recommendations:
Weight-bearing exercises
Activities like walking, jogging, dancing, and stair climbing stimulate bone formation by forcing the bones to work against gravity.
Resistance training
Using free weights, resistance bands, or body weight in exercises like squats and push-ups helps build muscle strength and bone density.
Balance exercises
Incorporating practices such as tai chi or yoga can improve stability and coordination, reducing the likelihood of falls.Engaging in a routine that combines these elements can lead to stronger bones and improved overall health. It’s recommended to aim for at least 150 minutes of moderate aerobic activity each week, complemented by strength training on two or more days.
Dietary Recommendations for Reducing Osteoporosis Risk
A well-rounded diet rich in essential nutrients can significantly lower the risk of osteoporosis. Certain minerals and vitamins, particularly magnesium and phosphorus, are critical for bone health. Here are some dietary recommendations:
Magnesium-rich foods
Include leafy greens (like spinach and kale), nuts (such as almonds and cashews), seeds (like pumpkin seeds), and whole grains (such as brown rice and oats) in your meals.
Phosphorus sources
Foods such as meat, poultry, fish, eggs, dairy products, and legumes are excellent sources of phosphorus, which plays a role in bone mineralization.
Calcium-rich foods
Incorporate dairy products like milk, yogurt, and cheese, as well as leafy green vegetables, almonds, and fortified foods like cereals.To enhance the effectiveness of these dietary choices, ensure a balanced intake of proteins, healthy fats, and a variety of fruits and vegetables. Staying hydrated and moderating caffeine and alcohol consumption can also contribute positively to bone health.
“Maintaining a diet rich in calcium, vitamin D, magnesium, and phosphorus is vital in reducing osteoporosis risk and promoting optimal bone health.”
Role of Lifestyle Choices in Osteoporosis Prevention
Making informed lifestyle choices plays a vital role in the prevention of osteoporosis. Factors such as smoking, alcohol consumption, and stress management significantly affect bone health. In this section, we will explore how these lifestyle choices influence bone density and overall health, and Artikel practical strategies to enhance bone strength through daily activities.
Impact of Smoking and Alcohol Consumption on Bone Density
Smoking and excessive alcohol intake are detrimental to bone density. Smoking interferes with the body’s ability to absorb calcium, a critical mineral for maintaining healthy bones. Studies indicate that smokers have a higher risk of fractures and a 20-30% lower bone mineral density compared to non-smokers. Alcohol also has a negative impact on bone health. Chronic alcohol consumption can lead to decreased calcium absorption and impaired bone formation.
The National Osteoporosis Foundation highlights that consuming more than two alcoholic drinks per day can increase the risk of osteoporosis. To mitigate these risks, reducing or eliminating smoking and limiting alcohol intake can greatly enhance bone strength. Embracing a smoke-free lifestyle and moderating alcohol consumption are critical steps toward maintaining healthy bones.
Stress Management and Its Effect on Overall Health
Chronic stress can lead to hormonal changes that negatively impact bone density. Elevated levels of the stress hormone cortisol may result in increased bone resorption, leading to a decrease in bone mass over time. Therefore, effective stress management techniques are essential for promoting overall health and maintaining bone strength.Several methods for managing stress include:
- Mindfulness meditation: Regular practice can lower cortisol levels and improve emotional well-being.
- Physical activity: Engaging in regular exercise not only helps in stress reduction but also promotes bone health.
- Breathing exercises: Simple techniques can help in calming the nervous system and alleviating stress.
- Social support: Building a support network can buffer the effects of stress and foster resilience.
Incorporating these techniques into daily routines can help mitigate stress effects, ultimately supporting better bone health.
Incorporating Weight-Bearing Activities into Daily Routines
Weight-bearing exercises are essential for maintaining and improving bone density. These activities force the body to work against gravity, stimulating the bones to strengthen. Implementing a plan to include such exercises in daily routines can significantly benefit bone health.A practical plan may involve:
- Walking: Aim for at least 30 minutes a day. Simple changes, like taking the stairs instead of elevators, can increase activity levels.
- Strength training: Incorporate resistance exercises twice a week, focusing on major muscle groups to enhance bone strength.
- Dancing: Fun and engaging, dance classes provide both cardiovascular benefits and weight-bearing activity.
- Yoga: Beyond flexibility, certain poses can enhance strength and balance while promoting bone health.
By finding enjoyable ways to stay active, individuals can make weight-bearing exercises a regular part of their lives, supporting optimal bone health throughout their lives.
Integrating Osteoporosis Prevention into Healthcare
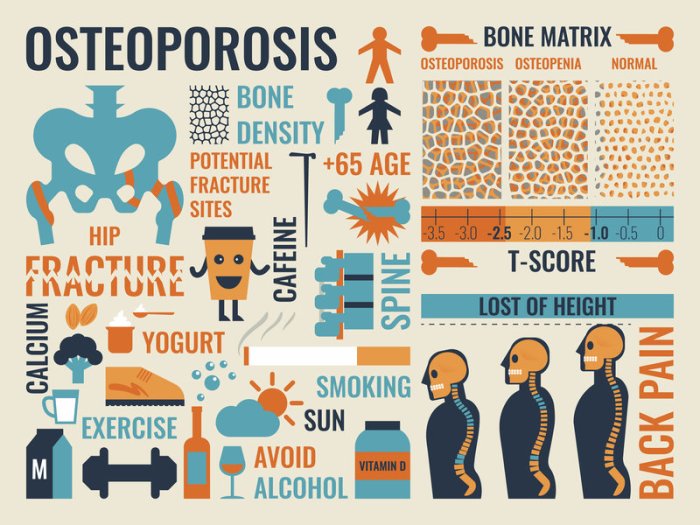
Osteoporosis prevention is an essential aspect of healthcare that requires proactive measures to ensure the health and well-being of individuals at risk. By integrating osteoporosis prevention strategies into healthcare systems, we can improve early detection and promote effective lifestyle changes among patients. This approach not only benefits individuals but also alleviates the broader healthcare system by reducing the incidence of fractures and related complications.
Importance of Regular Bone Density Screenings
Regular bone density screenings are crucial for the early detection of osteoporosis, allowing for timely interventions that can significantly alter the course of the disease. These screenings help identify individuals at risk before they experience fractures, which are often the first signs of osteoporosis. The National Osteoporosis Foundation recommends that women aged 65 and older and men aged 70 and older should undergo regular screenings.
Additionally, younger individuals with risk factors should also be considered for evaluation.
“Early detection through bone density testing can lead to more effective management and a better quality of life for patients.”
Healthcare professionals should emphasize the importance of these screenings to their patients, and the frequency of testing can vary based on individual risk factors. For instance, individuals with a previous fracture, family history of osteoporosis, or long-term use of corticosteroids may require more frequent assessments.
Community Awareness Programs Focused on Nutrition and Physical Activity
Creating community awareness programs that emphasize the importance of nutrition and physical activity for osteoporosis prevention is vital. These programs can engage the public in understanding how lifestyle choices impact bone health. Effective strategies might include workshops, seminars, and health fairs that promote the consumption of bone-healthy foods and encourage regular exercise.Educating the community about key nutrients such as calcium and vitamin D is essential.
- Calcium-rich foods include dairy products, leafy greens, and fortified foods.
- Vitamin D can be obtained through sunlight exposure and foods such as fatty fish and fortified cereals.
Incorporating physical activity into daily routines is equally important. Weight-bearing exercises, such as walking, jogging, or dancing, play a significant role in building and maintaining bone density.
Guidelines for Healthcare Professionals on Advising Patients
Healthcare professionals play a pivotal role in guiding patients toward effective lifestyle changes that prevent osteoporosis. Clear communication about the importance of healthy habits can enhance patient engagement and adherence to preventive measures.To aid healthcare professionals, the following guidelines can be considered:
- Encourage a balanced diet rich in calcium and vitamin D.
- Advise regular weight-bearing and muscle-strengthening exercises.
- Discuss the importance of avoiding tobacco and limiting alcohol consumption.
- Provide tailored recommendations based on individual risk factors and medical history.
Implementing these guidelines not only supports patients in making informed choices but also fosters a collaborative approach to osteoporosis prevention. By prioritizing education, healthcare providers can significantly enhance the awareness and understanding of osteoporosis within their patient populations.
Closing Notes

In summary, osteoporosis prevention is not just about individual choices but also about community awareness and healthcare support. By prioritizing bone health through proper nutrition, regular exercise, and proactive lifestyle changes, we can significantly reduce the risk of osteoporosis. Let’s commit to integrating these strategies into our daily lives and advocate for stronger health initiatives that support bone health for all.
User Queries
What are the best sources of calcium?
Dairy products like milk, cheese, and yogurt, as well as leafy greens, nuts, and fortified foods are excellent sources of calcium.
How much vitamin D do I need daily?
Most adults need about 600 to 800 IU of vitamin D daily, but it can vary based on age and health conditions.
Can I prevent osteoporosis entirely?
While you may not be able to prevent osteoporosis completely, adopting a healthy lifestyle can significantly reduce your risk.
Is weight training beneficial for bone health?
Yes, weight training is highly beneficial as it helps strengthen bones and improve balance, reducing the risk of fractures.
How often should I get bone density screenings?
It’s recommended to have bone density screenings every 1-2 years, especially for individuals with risk factors for osteoporosis.





